The APEX team believes in keeping communities healthy, which is why we are committed to exceeding the expectations of our partners. A limb preservation center may be in the form of an office-based endovascular lab, a freestanding or hospital-based wound care/hyperbaric center, or an ambulatory surgery center. APEX also offers a disease management program for payers, which focuses on saving limbs while reducing costs.
As high as 80% of non-traumatic lower limb amputations are due to complications of diabetes. The care to avoid amputation is fragmented. As a medical community, we need to provide comprehensive coordinated care to preserve limbs. The incidence of lower extremity amputation in patients with diabetes is significantly higher in patients with lack of access to specialists, lower socioeconomic backgrounds, and people of color. The medical community needs to be aware of the disparities and provide patients with the care needed to save limbs. Understanding the “Four Pillars of Limb Preservation” is key to providing this care.
Limb preservation goes beyond just treating individual symptoms; it involves a holistic approach that considers the entire patient, their medical history, and the interplay of various factors affecting limb health.
There are four pillars to build a comprehensive program to preserve limbs. These pillars include medical management, revascularization, wound care and management of diabetic neuropathy.
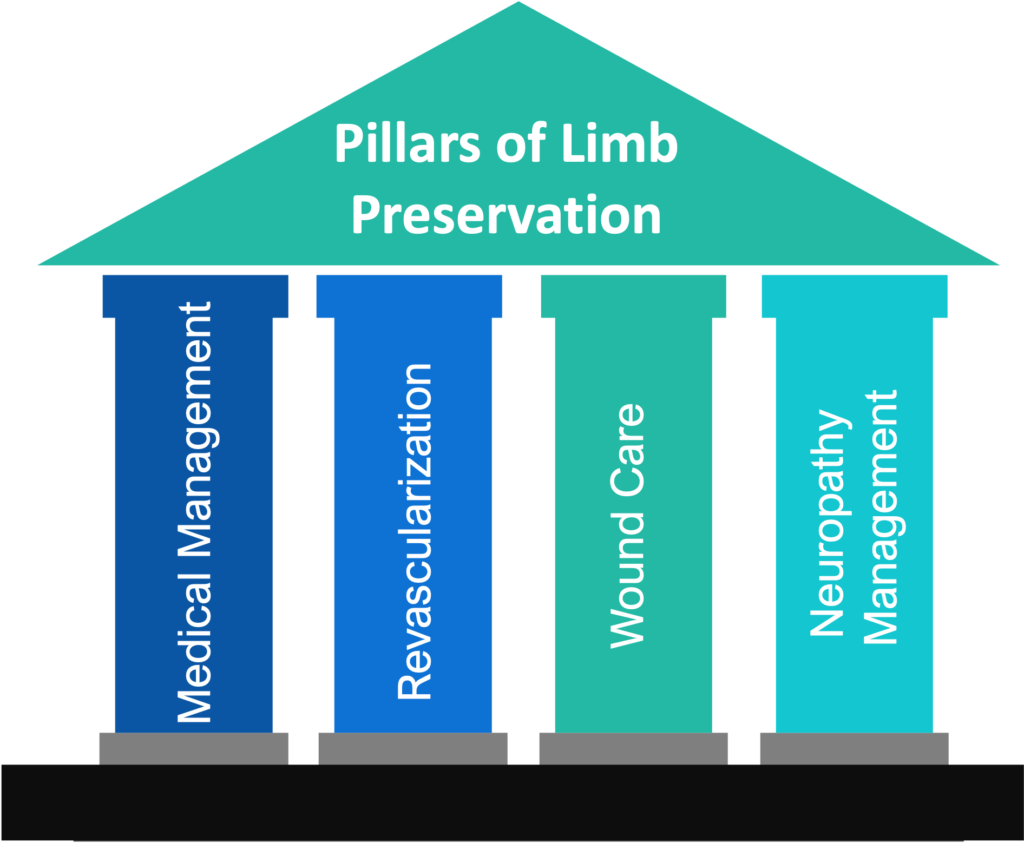
Any hospital system that wants to be a part of the LPCA network must meet certain requirements. The LPCA model is built on four pillars, namely medical management, revascularization, wound care and management of neuropathy. The traditional model of “Toe and Flow” (see Rogers et al, “Journal of Vascular surgery, 2010) is built for limb salvage. That means the limb is already compromised and if not treated in a timely manner will be lost.
Many hospital systems that have an amputation prevention center are designed to provide care under this model. The LPCA model includes “Toe and Flow” protocols and expands them to emphasize prevention as well as management of peripheral neuropathy which causes ulceration on the foot without patients being aware of the lesion.
LPCA emphasizes the need for a multispecialty, multimodality approach. This means that all physicians, who are part of the care plan should provide timely care to patients.
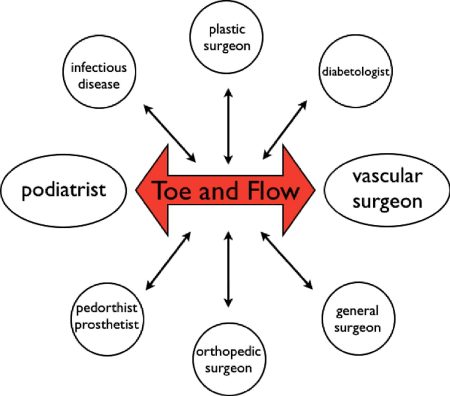
Multidisciplinary Team
In addition to the core vascular surgeon/interventional vascular specialist and surgical podiatrist, the following primary care and specialist physicians may be needed for comprehensive care of these patients:
OTHER REQUIREMENTS
It is vital to utilize an electronic medical record system that can provide key reports and track outcomes. The specialty center also can facilitate regional education, both professional and consumer, in an effort to make as many providers and patients aware of the service.
Most of the elements required to be part of the LPCA network already exist in many hospitals. Unfortunately, these elements frequently work in silos. Services like wound care and HBO, if not present, can be added, and where they are present, the services can be expanded to meet the LPCA criteria. APEX will help develop a multispecialty, multimodality collaborative approach to preserve limbs. Developing a limb preservation center can make a hospital the center of excellence in the community and the region in limb preservation. Adding a limb preservation center can also increase the number of patients seeking care at the host hospital. Significant number of these patients have other risk factors which include diabetes mellitus, hypertension and hyperlipidemia. Many of these patients also have coronary artery disease and renal impairment needing care. All these patients should be managed by the physicians affiliated with a limb preservation center.
Independent practitioners who have office-based labs or ambulatory surgery centers can add wound care and hyperbaric oxygen treatment to their practice and have agreements with other specialists to satisfy the requirements to be a part of Limb Preservation Centers of America.
Check back soon as more centers join the Limb Preservation Centers of America network. If you’re interested in becoming a member, reach out to learn more. We look forward to connecting with you!
Dr. Jain is Chief Medical Officer for Amputation Prevention Experts Health Network and founder of Limb Preservation Centers of America®. He is a board-certified vascular surgeon who has been intimately involved in the growth of office-based endovascular labs (OBLs) throughout the U.S. He is a founder of South Asian American Vascular Society, founding member of the Outpatient Endovascular and Interventional Society (OEIS) and a distinguished fellow of Society for Vascular Surgery (SVS). He was awarded Community Service award by Society for vascular Surgery. Dr. Jain has authored many widely-quoted papers and chapters and has written the book that serves as an expert guide in developing and operating an OBL, entitled “Office-Based Endovascular Centers” (Jain, K. M., 2019. Office-Based Endovascular Centers. Elsevier Health Sciences). He is the editor of forthcoming book “Essentials of lower limb preservation” being published by Cambridge scholars publishing.

The Limb Preservation Centers of America (LPCA) was the creation of a mission-driven vascular surgeon, Krishna Jain, MD, whose career has been dedicated to saving limbs. APEX Health Network develops and manages LPCAs, wound care and hyperbaric programs and also partners with doctors in developing and managing office-based endovascular centers and/or ambulatory surgery centers, all with a focus on limb preservation.
A wound care center treats chronic wounds, including diabetic foot ulcers, venous ulcers and pressure ulcers. A Limb Preservation Center places a focus on prevention and timely intervention to improve management of diabetic foot ulcers/infections and other limb-threatening conditions. In addition, our world-renowned limb preservation experts ensure that best practices are followed to avoid unnecessary major lower-limb amputations.
If you have any questions, or want to get started with an LPCA, please submit the form below.
Depending on space needs and which components of the program must be developed, the process can take anywhere from three to six months. Our team will work with you to identify your specific needs and come up with a timeline. We tailor the program to meet your needs.

© 2026 by Amputation Prevention Experts Health Network